NCLEX Respiratory Questions: COPD, Asthma, Pneumonia & PE Study Guide
If there is one principle that drives clinical nursing — and dominates nclex respiratory questions — it is this: Airway = Life. The respiratory system is the single highest-priority body system on the NCLEX-RN. A blocked airway kills in minutes. Without adequate oxygenation, every other system fails. That is why respiratory disorders nclex questions appear on virtually every exam, and why nurses answer them first when a patient is deteriorating. This guide covers the four most heavily tested respiratory conditions — COPD, Asthma, Pneumonia, and Pulmonary Embolism — with ABG interpretation, medications, priority nursing actions, mnemonics, and practice questions with full rationales.

Airway = Life: The Respiratory Priority Framework
The NCLEX is built around the ABCs — Airway, Breathing, Circulation. Respiratory questions test whether you know how to recognize impaired oxygenation fast and act before the patient collapses. Every intervention in this guide flows from one question: is this patient getting enough oxygen to their tissues? When the answer is no, everything else waits.
NCLEX Respiratory Basics: Physiology You Must Know
Before diving into specific diseases, lock in these foundational concepts that appear repeatedly in nclex rn respiratory questions. The lungs serve two functions: ventilation (moving air in and out) and perfusion (delivering oxygenated blood to tissues via the pulmonary circulation). Most respiratory pathology involves a disruption of one or both.
Key terms the NCLEX tests:
- V/Q Mismatch (Ventilation/Perfusion Mismatch): When ventilation and perfusion are not matched in lung units. In COPD and pneumonia, some alveoli are ventilated but not perfused (dead space); in PE, blood cannot reach ventilated areas. Both create hypoxemia.
- Hypoxemia: Low oxygen in the blood (PaO2 < 80 mmHg). Manifests as confusion, tachycardia, cyanosis, and restlessness.
- Hypercapnia: Elevated CO2 in the blood (PaCO2 > 45 mmHg). Causes respiratory acidosis. Found in COPD exacerbations and hypoventilation states.
- Hypoxic Drive: In patients with chronic CO2 retention (COPD), the stimulus to breathe switches from high CO2 to low O2. Giving too much supplemental oxygen can suppress this drive.
ABG Quick Reference for Respiratory Conditions:
| Condition | pH | PaCO2 | HCO3 | Interpretation |
|---|---|---|---|---|
| Normal | 7.35–7.45 | 35–45 mmHg | 22–26 mEq/L | Normal |
| Respiratory Acidosis | < 7.35 | > 45 mmHg | Normal/↑ (compensated) | Hypoventilation (COPD, opioid OD) |
| Respiratory Alkalosis | > 7.45 | < 35 mmHg | Normal/↓ (compensated) | Hyperventilation (anxiety, PE, early asthma) |
| Metabolic Acidosis | < 7.35 | Normal/↓ (compensated) | < 22 mEq/L | Sepsis, DKA, renal failure |
| Metabolic Alkalosis | > 7.45 | Normal/↑ (compensated) | > 26 mEq/L | Vomiting, NG suction, diuretics |
Use the ROME mnemonic for abg interpretation nclex questions: Respiratory Opposite (pH and PaCO2 move in opposite directions), Metabolic Equal (pH and HCO3 move in the same direction).
COPD on the NCLEX
Chronic obstructive pulmonary disease (COPD) encompasses emphysema and chronic bronchitis. The hallmark is irreversible airflow obstruction — this is the most critical differentiating fact between COPD and asthma. COPD results from years of inflammation, most commonly from smoking. By the time a patient is symptomatic, significant lung destruction has already occurred.
Classic NCLEX signs of COPD:
- Barrel chest — hyperinflation of the chest due to air trapping; the AP diameter equals the lateral diameter
- Pursed-lip breathing — a compensatory technique that creates back-pressure to keep airways open during exhalation and prevents alveolar collapse
- Tripod position — patient sits leaning forward with hands on knees to maximize the use of accessory muscles
- Diminished breath sounds with prolonged expiratory phase and expiratory wheezes
- Chronic productive cough (especially in chronic bronchitis), cyanosis (late sign), digital clubbing
In COPD exacerbation, administer controlled, titrated oxygen — typically starting at low-flow (1–2 L/min via nasal cannula) — and titrate to maintain SpO2 88–92%. Do not withhold oxygen if the patient is severely hypoxemic. Monitor closely for CO2 retention and signs of respiratory failure. Excess oxygen in COPD can worsen hypercapnia through multiple mechanisms including V/Q mismatch changes and the Haldane effect, not only hypoxic drive suppression. The NCLEX most commonly tests controlled oxygen delivery targeting 88–92% — not the standard 95%+ goal used in other patients.
Priority nursing actions for COPD exacerbation:
- Position in high-Fowler's or tripod position to ease breathing
- Administer low-flow O2 (1–2 L/NC); monitor SpO2 — target 88–92%
- Administer prescribed bronchodilators (albuterol via nebulizer or MDI)
- Teach pursed-lip breathing and diaphragmatic breathing techniques
- Encourage smoking cessation (most important modifiable factor)
- Monitor for signs of respiratory failure: worsening confusion, CO2 narcosis
COPD medications the NCLEX expects you to know:
- Tiotropium (Spiriva) — long-acting anticholinergic bronchodilator; once-daily inhalation; reduces exacerbation frequency; a maintenance (not rescue) medication
- Albuterol (ProAir, Ventolin) — short-acting beta-2 agonist (SABA); the rescue inhaler for acute bronchospasm; onset within 5 minutes
- Ipratropium (Atrovent) — short-acting anticholinergic bronchodilator; often combined with albuterol (Combivent) for acute exacerbations
- Corticosteroids (prednisone, methylprednisolone) — reduce airway inflammation during exacerbations; oral or IV; not recommended for long-term daily use due to side effects (immunosuppression, osteoporosis, hyperglycemia)
The most tested COPD concept is the oxygen rule. The NCLEX expects controlled oxygen for COPD — usually starting low-flow, titrated to SpO2 88–92%. A second high-yield theme is pursed-lip breathing — know what it does and why the patient does it. Third: COPD is irreversible. Asthma can improve with treatment. COPD cannot. If a question asks which patient will fully recover, it is not the COPD patient.
A nurse is caring for a patient with COPD who has an SpO2 of 84% and a respiratory rate of 28/min . Which action should the nurse take first?
For a COPD patient with low SpO2, apply low-flow oxygen (1–2 L/min via nasal cannula) and titrate to a target SpO2 of 88–92% . High-flow oxygen is avoided because it can worsen CO2 retention by suppressing the hypoxic respiratory drive.
Asthma on the NCLEX
Asthma is a reversible obstructive airway disease characterized by bronchoconstriction, airway inflammation, and increased mucus production triggered by allergens, cold air, exercise, or irritants. Unlike COPD, asthma attacks can resolve completely with appropriate treatment — reversibility is the defining characteristic. Understanding this distinction is essential for med surg respiratory nclex questions.
Status asthmaticus is a severe, prolonged asthma attack unresponsive to standard bronchodilator therapy. It is a medical emergency. The most ominous sign is a silent chest — on auscultation, you hear NO breath sounds, not even wheezing. This means the patient is moving so little air that there is nothing to hear. Silent chest = impending respiratory arrest. Call the rapid response team immediately and prepare for intubation.
Classic NCLEX signs of asthma exacerbation:
- Wheezing (high-pitched musical sounds) — predominantly expiratory
- Dyspnea, tachypnea, tachycardia
- Use of accessory muscles, nasal flaring (especially in children)
- Peak expiratory flow rate (PEFR) below 80% of personal best — indicates significant obstruction
- Hypoxemia on pulse oximetry; early ABG shows respiratory alkalosis (hyperventilation); late/severe ABG shows respiratory acidosis (fatigue)
- A rising PaCO2 in a severe asthma patient is a danger sign — the patient is tiring
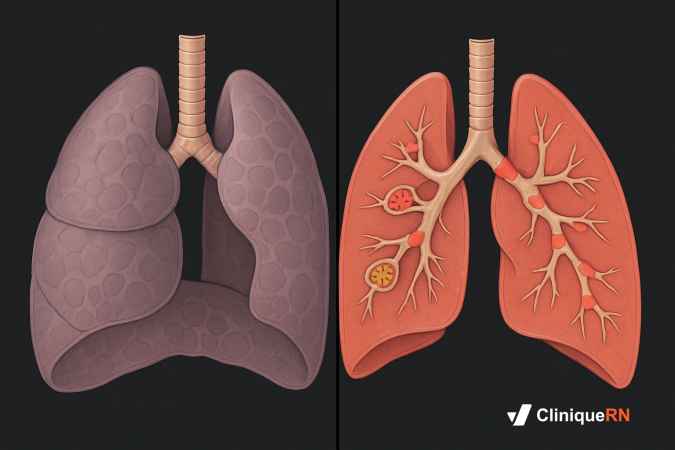
COPD vs. Asthma: The Comparison the NCLEX Loves
COPD and asthma are both obstructive lung diseases, but they differ in reversibility, onset, triggers, and oxygen management. Memorize this comparison — it appears on virtually every NCLEX respiratory review. COPD: irreversible, barrel chest, hypoxic drive, cautious low-flow O2. Asthma: reversible, triggered by allergens, SABA first, standard O2 unless severe.
COPD vs. Asthma Comparison Table:
| Feature | COPD | Asthma |
|---|---|---|
| Reversibility | Irreversible | Reversible |
| Typical onset | Gradual (years of smoking) | Variable (any age; often childhood) |
| Common triggers | Smoking, infection, pollution | Allergens, cold air, exercise, stress |
| Breath sounds | Diminished; prolonged expiration; expiratory wheeze | Expiratory wheeze; silent chest in severe attack |
| Chest appearance | Barrel chest, hyperinflation | Normal between attacks; chest tightness during |
| O2 approach | Controlled/titrated O2; target SpO2 88–92% | Titrate O2 to SpO2 93–95% (adults/adolescents) |
| Primary treatment | Bronchodilators, smoking cessation, tiotropium | SABA (rescue), ICS (maintenance), steroids |
Priority nursing actions for acute asthma:
- Position in high-Fowler's; allow the patient to assume a position of comfort (often tripod or sitting upright)
- Administer SABA (albuterol) via nebulizer or MDI with spacer — this is ALWAYS the first medication
- Apply supplemental oxygen; titrate to maintain SpO2 93–95% in adults/adolescents (94–98% in children 6–12 years)
- Administer corticosteroids (IV methylprednisolone or oral prednisone) to reduce inflammation
- Monitor peak flow before and after bronchodilator treatment
- Auscultate for return of breath sounds after treatment — absence of wheeze after treatment suggests improvement; absence before treatment may signal silent chest
- Educate on avoiding triggers, using peak flow meter at home, and the difference between rescue and maintenance inhalers
The first drug in asthma is always a SABA (albuterol). Corticosteroids follow — they reduce inflammation but are not fast-acting enough to open airways in an acute attack. Know the difference between rescue inhalers (SABAs — used in acute attacks) and controller inhalers (inhaled corticosteroids — used daily for prevention). The silent chest must be memorized as a critical danger sign.
A patient with asthma is brought to the emergency department in acute distress. On auscultation, the nurse notes no breath sounds in the bilateral lung fields. The patient's SpO2 is 88% and they are using accessory muscles . Which is the nurse's priority action?
A silent chest in an asthma patient is a sign of status asthmaticus and impending respiratory arrest . The nurse must notify the rapid response team immediately — this is a medical emergency that cannot be managed alone or by waiting to reassess.
Pneumonia on the NCLEX
Pneumonia is an inflammatory infection of the lung parenchyma (alveoli and surrounding tissue) caused by bacteria, viruses, or fungi. It is one of the most commonly tested respiratory disorders nclex students encounter, and it appears across multiple client need categories — from infection control to priority nursing to delegation. Pneumonia is a leading cause of infectious disease morbidity and mortality in the United States — particularly in older adults and hospitalized patients — which is why the NCLEX treats it as high-stakes.
Community-Acquired vs. Hospital-Acquired Pneumonia:
- Community-acquired pneumonia (CAP) — acquired outside the hospital or within 48 hours of admission. Most common causative organism: Streptococcus pneumoniae. Treatment: amoxicillin or a macrolide (azithromycin) for outpatients.
- Hospital-acquired pneumonia (HAP) — develops 48+ hours after hospital admission. More likely caused by gram-negative organisms (Pseudomonas, Klebsiella) and MRSA. Requires broader-spectrum IV antibiotics. Associated with mechanical ventilation (VAP — ventilator-associated pneumonia).
Classic NCLEX signs of pneumonia:
- Fever, chills, night sweats
- Productive cough with purulent, rust-colored, or blood-tinged sputum
- Pleuritic chest pain (sharp pain on inspiration — the inflamed pleura rubs against the chest wall)
- Crackles (rales) on auscultation — the hallmark finding, especially at the lung base
- Consolidation on chest X-ray — one of the most distinctive pneumonia NCLEX findings (opaque, "white-out" area in the affected lobe)
- Decreased breath sounds over the affected area; dullness to percussion
Priority nursing interventions for pneumonia:
- Elevate the head of bed to 30–45 degrees at minimum — this improves lung expansion and reduces aspiration risk
- Positioning for oxygenation: Place the patient with the affected (sick) lung UP to maximize perfusion to the healthy lung. This is the opposite of what many students expect — the unaffected lung DOWN receives better blood flow, improving overall gas exchange. This is a KEY NCLEX favorite.
- Encourage incentive spirometry 10 times every hour while awake — prevents atelectasis and promotes alveolar expansion
- Encourage fluids (2–3 L/day unless contraindicated) — thins secretions and makes them easier to expectorate
- Encourage deep breathing, coughing, and early ambulation when able
- Administer prescribed antibiotics promptly — the first dose should be given as soon as possible after blood cultures are drawn
- Monitor vital signs for fever trends and respiratory status (RR, SpO2)
- Implement droplet precautions if the causative organism warrants
Aspiration pneumonia results from inhaling oropharyngeal secretions, food, or gastric contents into the lungs. High-risk patients: those with dysphagia, decreased level of consciousness, nasogastric tube placement, recent extubation, or post-stroke. Priority: keep HOB elevated, check tube placement before each feeding, perform oral care every 2–4 hours in intubated patients.
Pneumonia is a common precipitant of sepsis. Monitor for: temperature > 38.3°C or < 36°C, HR > 90 bpm, RR > 20/min, altered mental status, and systolic BP < 90 mmHg. Early sepsis recognition → blood cultures → broad-spectrum antibiotics within 1 hour → IV fluids. Delay increases mortality.
The two most tested pneumonia concepts are: (1) positioning — affected lung UP for oxygenation is counterintuitive and therefore a frequent NCLEX distractor; (2) incentive spirometry — the nurse should teach its use and encourage 10 breaths per hour. Also know that crackles are the hallmark breath sound and consolidation is the hallmark X-ray finding. Aspiration risk and droplet vs. standard precautions are commonly tested in infection control questions.
A nurse is caring for a patient with left lower lobe pneumonia . The patient has an SpO2 of 90% on room air. Which nursing action best improves this patient's oxygenation?
For unilateral pneumonia, position the patient with the healthy lung DOWN to maximize perfusion to functional alveoli. For left lower lobe pneumonia, this means right side down (left lung up) — the counterintuitive positioning that the NCLEX frequently tests.
Pulmonary Embolism on the NCLEX
Pulmonary embolism (PE) occurs when a thrombus (usually from a DVT in the lower extremities) travels through the venous system, through the right heart, and lodges in the pulmonary vasculature, obstructing blood flow to a section of lung. PE is one of the most critical respiratory emergencies the NCLEX tests because the priority actions follow a strict sequence — and getting the order wrong could mean choosing a wrong answer.
Virchow's Triad — the 3 risk factors for DVT and PE:
- Venous stasis (immobility) — prolonged bedrest, long flight, hospitalization, post-operative state
- Hypercoagulability — pregnancy, OCP use, cancer, inherited clotting disorders (Factor V Leiden)
- Vessel wall damage — surgery, trauma, IV catheter insertion
Classic PE triad on the NCLEX:
- Sudden onset dyspnea — the most consistent presenting sign; may occur at rest
- Pleuritic chest pain — sharp, stabbing pain that worsens with inspiration
- Tachycardia — the heart compensates for decreased cardiac output by increasing rate
Additional signs: anxiety, diaphoresis, hemoptysis (blood in sputum), decreased SpO2, pleural friction rub. D-dimer is a highly sensitive screening test — a negative result can help rule out PE in patients with low or intermediate clinical probability, but it is not used alone in high-risk patients. CT pulmonary angiography is the gold standard diagnostic.
PE Priority Actions: The Sequence That Wins NCLEX Questions
Pulmonary embolism is a cardiovascular emergency masked as a respiratory problem. The priority action sequence matters: Oxygen FIRST to treat hypoxemia → notify the provider → prepare for anticoagulation (IV Heparin). Getting this order right is the difference between a correct and incorrect answer on the NCLEX. Never massage a swollen extremity — you could dislodge a clot.
Priority nursing actions for PE — in order:
- Oxygen first — apply high-flow O2 (100% via non-rebreather); correct the life-threatening hypoxemia immediately
- Notify the provider — this is an emergency; the patient needs immediate diagnosis and anticoagulation orders
- Elevate HOB — ease the work of breathing
- IV access and labs — D-dimer, CBC, coagulation studies, troponin (for right heart strain)
- Anticoagulation — anticoagulation is the cornerstone of PE treatment; IV Unfractionated Heparin is commonly used in acute hospital settings because it acts quickly and can be reversed; medication choice depends on provider order, patient stability, renal function, and bleeding risk — the nurse does not select the agent; does NOT dissolve the existing clot (fibrinolytics do that, in massive PE)
- Monitor for hemodynamic stability — massive PE can cause obstructive shock; watch BP, HR, and mental status
What NOT to do — Critical NCLEX Points:
- Never massage a DVT — massage can dislodge the thrombus and turn a DVT into a PE
- Never use aspirin alone for anticoagulation in PE — aspirin affects platelet function but does not prevent venous thromboembolism progression
- Do not massage the affected extremity — massage can dislodge the thrombus; do not apply compression devices or stockings unless specifically prescribed — selected patients with DVT may use compression for symptom relief, but this requires a provider order and is not an independent nursing action
- Never have the patient ambulate when an acute DVT or PE is suspected and not yet anticoagulated
The exam loves to test the sequence of actions: oxygen comes before calling the doctor in priority questions because oxygenating the patient is the most immediately life-saving intervention a nurse can do independently. Know Virchow's Triad cold — any question that involves a post-op patient, a patient on a long flight, or a pregnant patient with sudden dyspnea should make you think PE. D-dimer is a sensitive but not specific test — it is elevated in many conditions.
A post-surgical patient reports sudden onset of dyspnea and sharp chest pain with breathing . The nurse notes HR 118 bpm and SpO2 87% . Which is the nurse's first action?
With an SpO2 of 87%, the nurse's first action is to apply high-flow oxygen via non-rebreather mask . ABCs always come first — oxygenate the patient before calling the team or initiating diagnostics. This is the nurse's first independent life-saving intervention.
ABG Interpretation Quick Reference (ROME Method)
ABG interpretation is a high-yield skill for nclex rn respiratory questions. Use the ROME method to identify if the problem is respiratory or metabolic, and whether compensation has occurred.
| Step | Normal Range | If Abnormal |
|---|---|---|
| 1. pH | 7.35–7.45 | < 7.35 = Acidosis; > 7.45 = Alkalosis |
| 2. PaCO2 (Respiratory) | 35–45 mmHg | > 45 = Respiratory Acidosis; < 35 = Respiratory Alkalosis |
| 3. HCO3 (Metabolic) | 22–26 mEq/L | < 22 = Metabolic Acidosis; > 26 = Metabolic Alkalosis |
| 4. Compensated? | pH within normal range | If pH normal but PaCO2 and HCO3 both abnormal = fully compensated |
Respiratory conditions and expected ABG findings:
- COPD exacerbation: pH ↓ (acidosis), PaCO2 ↑ (CO2 retention), HCO3 ↑ (chronic compensation) → Compensated Respiratory Acidosis
- Acute asthma (early): pH ↑, PaCO2 ↓ (hyperventilation) → Respiratory Alkalosis
- Acute asthma (severe/late): pH ↓, PaCO2 ↑ (patient fatiguing, can't move air) → Respiratory Acidosis — a danger sign
- Pulmonary embolism: pH ↑, PaCO2 ↓ (hyperventilation due to hypoxemia) → Respiratory Alkalosis
- Pneumonia (severe): pH ↓, PaCO2 ↑ (hypoventilation from pain/fatigue) or metabolic acidosis if sepsis develops
Respiratory Mnemonics to Remember the Priorities
Mnemonics lock in complex clinical information quickly. Use these for nclex respiratory questions:
Barrel chest from hyperinflation. Bronchospasm causes the wheeze. Give controlled, titrated O2 — start low-flow and target SpO2 88–92%. Uncontrolled high-flow O2 can worsen CO2 retention in COPD. Pursed-lip breathing buys time between exacerbations by preventing airway collapse.
In an acute asthma attack, SABA (albuterol) is the FIRST medication. Steroids follow to reduce inflammation but take hours to work. A silent chest means no air is moving — escalate immediately. Peak flow below 50% personal best = severe attack.
Affected lung UP for oxygenation. Fluids help thin secretions. Watch for fever spikes and signs of sepsis (tachycardia, hypotension, altered mental status). Incentive spirometry every hour while awake prevents atelectasis.
Sudden Dyspnea is the cardinal sign. D-dimer is the screening test. DVT risk factors (Virchow's Triad) are the backstory. Priority: O2 → notify provider → Heparin. Never massage the DVT site. Never use aspirin alone.
When a respiratory NCLEX question asks "what does the nurse do first?" — if the patient has respiratory distress and a low SpO2, applying oxygen is typically the nurse's first independent action. Oxygenating the patient is the most immediately life-saving intervention within nursing scope. Call the provider after securing the airway and positioning the patient. Exception: if the patient is unresponsive, pulseless, or in impending arrest, call for help and activate the emergency response simultaneously — do not delay rescue efforts to apply oxygen alone.
NCLEX Success Tip